Piriformis Syndrome & Back Bain
Piriformis syndrome is a very common diagnosis and self-diagnosis when you happen to look up symptoms that can also commonly be caused by sciatica. So what exactly is piriformis syndrome, what are the ins and outs of the anatomy around the piriformis muscle and what do we think a more likely cause of these symptoms is?
Where Is The Piriformis Muscle?
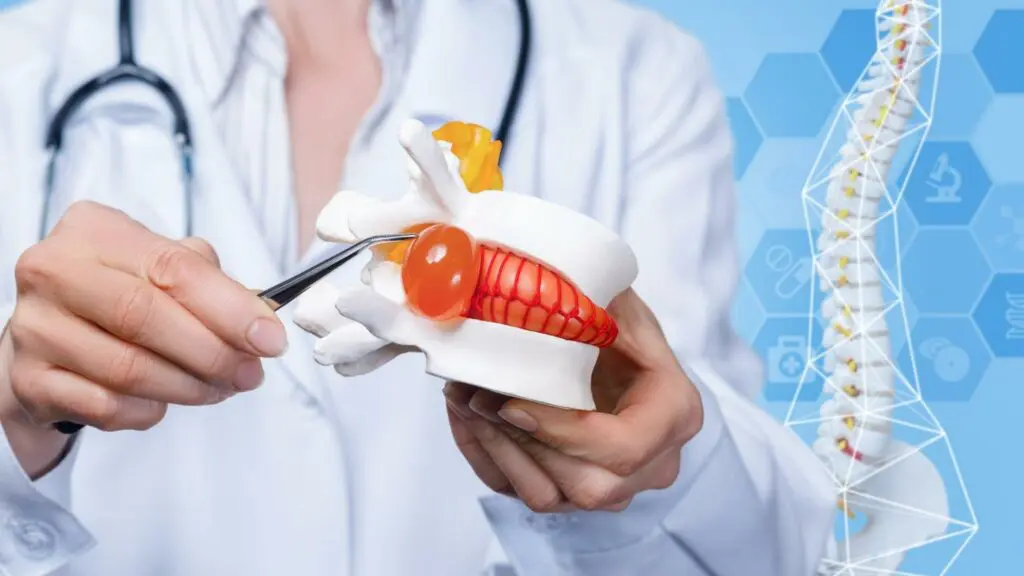
In the video at the top of the page, we show you the anatomy of the hip, including the hip rotator muscles. The piriformis muscle sits on top of the sciatic nerve, which is commonly why it is blamed for that typical pain or ache in the buttocks. However, this area is very well supported, with lots of muscles that work in synergy with one another to help the hip and legs function effectively. All of the muscles in this area have the same nerve supply, meaning they’re all controlled by the same nerve: the sciatic nerve. If this nerve is irritated at its root, it’s going to cause symptoms including muscle spasm, aching, pins and needles sensations, stabbing or burning pain. These symptoms are going to occur anywhere from the lower back itself where the nerve root is located or anywhere along the nerve itself, i.e. into the buttocks or down the back of either legs and into the feet. A specific muscle can only be the potential cause of a problem when it is able to be isolated and overstrained. If someone were to ask you to engage your piriformis muscle, you’re not going to be able to do so as the muscles in this area work together.
What If You’ve Been Told You Have Piriformis Syndrome?
If you’ve been previously told the piriformis muscle is the problem, try and visit another practitioner for a second opinion. A practitioner that’s going to take a look at the spine with imaging if necessary to have a look at the lower back instead is going to be worthwhile. An upright X-ray is going to indicate whether there is any compression or lack of disc space evident in the spine as well as give an insight into the positioning of your spine. The positioning is going to explain why the problem has occurred in the first place, and the right practitioner should also be giving you tools to help rectify this as well. A common counter argument amongst practitioners is to point out that the surpraspinatus tendon can be injured on its own, so therefore so can the piriformis muscle, however the supraspinatus tendon has a very unique blood supply system. This makes it unable to be compared to any other area of the body in that respect. Outside of a second opinion, you can treat the problem as a lower back issue to understand what kind of rehabilitation can be done.
Our Back In Shape membership area is designed for any kind of back pain, including the sciatic pain that is commonly misdiagnosed as piriformis syndrome. Looking towards the lumbar spine instead, our membership area recommends the right stages of rehabilitation for your severity of pain. For very severe pain, the Phase 1 rehabilitation provides a two-step, inflammation relieving protocol, stretches that help to improve the function of your lower body, as well as a core-engagement exercise to teach you how to recruit these muscles so that you’re ready to do this in the later strengthening phases. Phase 2 is designed for anyone who has been doing the Phase 1 for a couple of days already, or can walk around for 15 minutes or more (with or without pain). This section starts to integrate exercises that challenge the lower body, core and back in a low-intensity way. These are less strenuous than the day-to-day activities you would do around the house, so it’s vital that you don’t skip them in favour of rest. Phase 3 furthers the strengthening by introducing added resistance and posture correcting exercises, so that you can train your body for general health and wellbeing, as well as supporting your spine.