
Which Is Better For Back Pain & Sciatica, MRI or X-Ray?
When it comes to imaging for lower back pain, the common belief held by many is that MRI’s are the superior imaging technology. This of course is correct, however just because it is the superior imaging technology, doesn’t necessarily mean that it is optimal for back pain. This week we follow on from the last release on imaging and discuss what would be the best imaging for lower back pain.
To begin however we need to first refine the objective, something like the following:
What is the best imaging to help a patient who is suffering from lower back pain make improvement and work to improve their symptom picture and injury profile.
We could have an additional question:
What is the best imaging if we want to do surgery on the back, or deliver injections to the back.
You see, the quality of the question is what dictates the answer we give. Also note the second question had nothing to do with your back pain, or understanding it better…
Fundamentally the low back is a load bearing structure. When the back fails and becomes injured, it is a failure to bear load that is at the root cause. Something has gone, and perhaps it was weakness in an awkward position, cumulative low grade bombardment over years, or a one off extreme load bearing event. But the fact remains; back injuries are a failure to handle a loaded spine in the overwhelming majority of cases.
Following on from this, the loading of an injured back is most frequently, and unsurprisingly, a major factor in aggravation. It could be the simple presence of load itself, it could be the presence of load with movement, but the simple fact remains. Many with back injuries, feel more pain with loading, and less when load is removed. This could be through a function of letting go of a carried item (load) or adopting a position that decreases load on the injured part of the spine. There are some additional peculiarities in this department but we needn’t cover those here.
If we draw the parallel to a bucket, the bucket is designed to bear load in the way it contains water or cargo within. The bucket would fail if there were to become a weakness in this ability to contain the cargo, perhaps because a joint between the side and the bottom of the bucket has been damaged. To understand where the bucket is failing and needs repairing, we would have the good sense to expedite the process by filling the bucket with water and examining what happens when the bucket is forced to carry out its role, bearing the load of cargo. You would immediately see the leak, or if the contents were solid, perhaps a bowing where the breakage was as it is strained by the load.
In short, you can quickly appreciate what’s wrong, and then formulate a fix when looking at the structure when it is carrying out its main role. The spine is no different. Looking at the spine should be done, for maximum benefit, within the context the spine is used daily, upright and load bearing as a bare minimum. We’ll cover this more later.
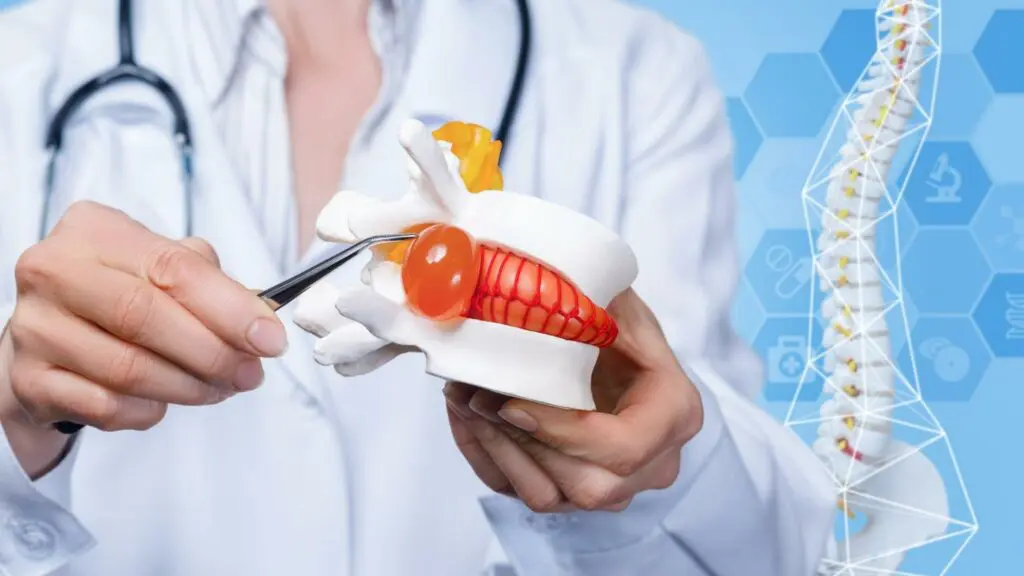
Is MRI imaging the best form of diagnostic imaging for the lower back?
Firstly, with MRI technology, we have to acknowledge the time it takes to capture the image. This is not like a photograph, it involves 30 to 60 minutes still in the MRI machine in order to gain images that are useful. Movement during this time can create issues so it is vital that we are in a position to increase the likelihood of a good image.
You might be surprised to know that there are standing MRI machines. But as you can imagine, taking someone in pain and asking them to stand still for a prolonged period of time makes it very difficult to get a useful image, not to mention that it would likely be prohibitively painful for many to endure such a confined stand to attention. Aside from this, upright MRI imaging is very expensive and generally speaking something you would have to fund privately, if you were to be fortunate to be located near to one of the few cities which have them.
This leaves us with the more common case of the lying down MRI, a position that many find a lot more pleasant than sitting or standing for 30 to 60 minute duration. So why is this the go to?
The primary use of the MRI imaging is to get an intimate understanding of the tissues in the low back with a view to inform next steps. The next steps are important as they explain the routine choice of MRI as the preferred imaging techniques for back pain. Typically, within the NHS in the UK, you’re being referred for MRI because you’ve had little success with prior measures: pain killers, doing nothing, physiotherapy, etc. The next options are going to be injections and surgery. Injections astoundingly can sometimes be referred for before imaging which boggles the mind but we won’t go there today…
If surgery is the consideration for the next step, then an MRI starts to make sense, it gives the surgeon the information on precisely which bit can be removed in the hope of helping symptoms. The big flaw here however, is that so often the MRI does not add a significant degree of usable information other than precisely which bit of disc could be removed or which bit of bone spur shaved down. Often we knew already ahead of the MRI that the injury was in that region. For example an L5/S1 disc injury, this MRI only gives the additional detail but this is not particularly useful for the individual and their daily life or informing rehabilitative exercises.
X-Ray Imaging For Lower Back Pain
If we contrast the load bearing X-ray image, this is much more pleasant for the patient, it also allows valuable insight which informs the processes going forwards and in the right hands, can provide information to further the patient’s understanding of their own body. Granted the tissues that we see on the X-ray for a lower back injury are only the bone. We can see degenerative changes in the bone, breaks, and other changes associated with trauma or degenerative processes. We unfortunately do not directly see the disc which is one of the major criticisms. However, we do see the space the disc should occupy, and therefore can make deductions about its condition.
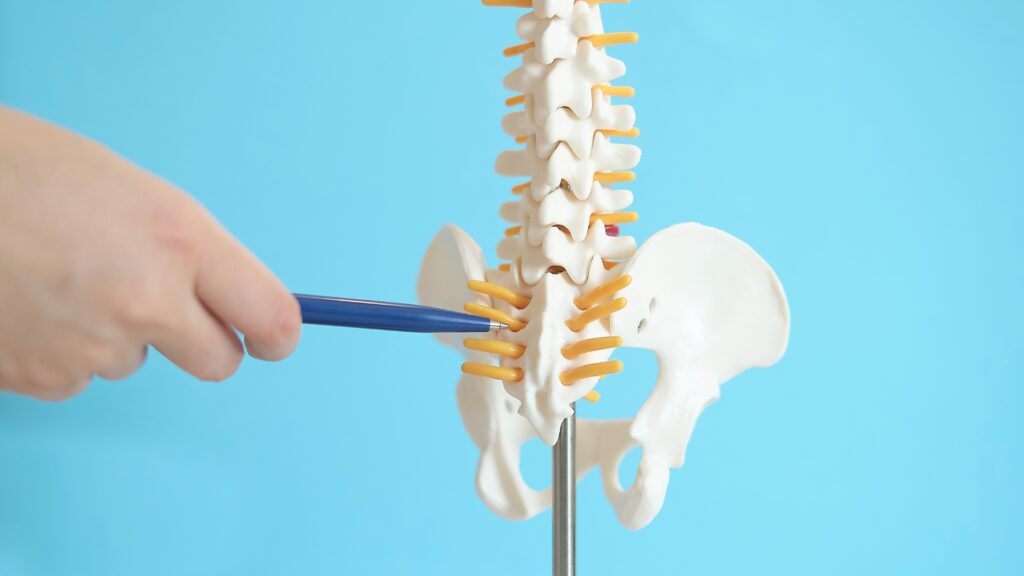
The important distinction here is that we can easily see the spine in its load bearing capacity. We can get an idea of the specific health of a suspected injured segment as it is used. Let us again propose the L5/S1 disc bulge. We see the approximate status of this disc space, perhaps the gap between L5 vertebral body and S1 reduced, indicating dysfunction at the level. We can also see how the overall spine loadbears:
How does that Lumbosacral junction sit within the context of the whole spine?
How does that spine balance in the standing position?
Is there a loss or increase of curve, if so how much precisely?
Is there an anterior or posterior tucking of the pelvis, and if so, how much, precisely?
Are there any short legs or pelvic tilts that are present, again precisely?
Much of the significant inaccuracy of a physical examination can be eliminated on the standing X-Ray. We can clearly see the best position this person is able to adopt, standing erect. If there are issues, such as a flattened lordosis, we can understand how that will affect activities like sitting. We can start to appreciate the sorts of strain this person’s back is under on a daily basis. These implications can then be relayed to the patient in a way that empowers them. Perhaps some of these things cannot be changed, but some can. Those that cannot be changed, can be compensated for.
Comparison of the imaging techniques for lower back pain
Ultimately neither set of imaging negates the need for you to build support for your back, through resistance training, to keep your hips flexible and strong, and have strategies to offset the many unhealthy ways we must use our bodies on a daily basis. As we discussed last week, those of you waiting for imaging to move forwards are making a mistake in 99.9% of cases.
When it comes to the both options for imaging, they can be a great tool to help empower the patient, gaining an understanding of how their own body works, and the implications their actions, lifestyle and other factors have on their back with reference to the injury but also to their long term back health.
MRI imaging gives you an insight into the minute detail of the soft tissues, however, this level of detail is often useless to the individual down to the fact that they cannot affect these things. The only practitioner that can meaningfully make use of such minute detail is the surgeon who can plan the injection or surgical intervention. However, without the load of gravity on the spine, things get missed.
On more than one occasion in the clinic, we’ve seen patients with MRI imaging have what looks to be a disc bulge or herniation and nothing more, only to find that the load bearing X-ray imaging reveals that disc bulge is at the level where a spondylolisthesis is present. This little detail has huge implications for the perceived course of action and the likely success of surgical interventions, to risk being ignorant of this, makes little sense.
Having the load bearing X-Ray imaging for your back pain, you can get a much more nuanced understanding of how this injury exists within a spine, that exists within the back of a person who carries out their daily lives. The nuance here allows you to have infinitely more impactful discussions with patients and them to have a much greater understanding of their own body and how to move forwards.
Spinal mechanics can be observed much more accurately and ultimately this makes for greater positive benefits for the patient. Quite often it leads to a more positive outlook for the patient too as they feel part of the solution as opposed to the alternative MRI based route.
Ultimately these are just tools though, they do not replace the need for us all to go about our daily lives in ways that are more healthy and to devote a small amount of time each week to working on our bodies through resistance training and targeted flexibility work.







Hi
I had an L2/L3 discectomy last week and have previously had spinal fusions L4-S1 and L3-L4. Long story short was a nurse and suffered multiple back injuries which resulted in my being unable to walk prior to each surgery.
The surgeon was very clear with me that I need to be really careful as all L2/L3 is carrying an enormous load due to the fusions. Have had some exercises on discharge which include knee to chest exercises.
When do you think I should restart phase 1 including towel stretch (have been advised to avoid extension for now). I never quite managed to get to phase 2 as the disc herniation was very large with some cord compression so discectomy was emergency.
Have lived with back pain for over 30 years having had my first serious injury in 1992 when manual handling training for nurses was somewhat lacking
Hey Jojo,
Thanks for the comment, That’s spot on and all the more important that you work on providing stability to the lower back! You’re in the right place, The towel will not be extending but rather supporting the natural spine position – compared to a “cobra” which CERTAINLY IS spinal extension. We would always advise against the knees to chest, especially given your information above – although they are nearly always recommended. We will go through this in more detail for you on the LIVE session on Wednesday PM (5:30pm UK time) so do try to make that!
Thank you – I will join the live session on Weds
It’s a pleasure, we just approved you in the group, do check out some of the recent comments in there as there are some which are very relevant to your comment and recent surgery which i think you’ll find helpful. (member comments and our replies).
Good Afternoon Michael,
Wondered if you could comment on this. As I may have mentioned before, I had an XRay while in the US, which identified anterolisthesis of L4 on L5. On looking at the Xray the shift is approx. 25% (Grade 1). The Chiropractor that referred me for an XRay (standing position), confirmed a 25% shift based on the Xray. However, what is confusing me is that in the Radiologist’s report he states “there is approximately 7mm of anterlisthesis of L4 on L5”. This I find confusing, since a 7mm shift across the diameter of L5 to me would be significant. Your comments would be much appreciated.
James
Good Afternoon Michael,
Not to worry about my query. I have managed to resolve it.
Thanks anyway.
James
Hi there James,
thanks for the question, Fundamentally they’re saying similar things, just one is a more specific measurement if you will 🙂 As a grade 1 would be a different “mm” measurement on a 6ft 4 male, compared to a 5 ft female – so the grading works better than a mm amount if that makes sense?
Hi Michael,
Thanks for your response. Makes sense, Grade 1 it is 0 -25%.
James
I am due to have surgery for a herniated disc at L4-L5 this week. What exercises should I do and when should I start doing them?
My wife who was a physio always told me that I had no lordosis in my lumbar area, but I never realised how much this could affect my back problem. Should I be discussing this with my surgeon?
Nigel Gray
Thanks for the question, It is likely that this has been a factor over time as it loads the discs a lot more, however, with the specific question you really want to discuss with your surgeon his/her timeframes for when you’ll be back at “normal activities” then compare those activities to the Phase 2/3 exercises and make the decision from there 🙂